TAYLOR’S JOURNEY
JEFF BROWN
Tempe, Arizona
We intended to share our story sooner, but as we all are aware 2020 changed everyone’s plans, including a delay to the next phase of Taylor’s journey. It felt incomplete to share without some positive long-term outcome.
Back to the beginning, Taylor always excelled at school and was a self-motivated hard worker. Achievement came naturally to her and she had big plans for the future. We are not sure when her major medical issues first arose, but we suspect she was dealing with some level of it for quite a long time before the obvious signs appeared.
Taylor left high school and went on to study engineering at Arizona State University pulling the typical college student burn-the-candle-at-both-ends lifestyle. In her junior year (2016–2017), our first overt signs of trouble appeared. We noticed she would be sleeping in the afternoon each day and was having a lot of nausea. For a while we chalked the tiredness up to crazy college hours, trying to get all her work in, and contribute to the research lab where she worked. In retrospect, we have realized Taylor would frequently get very tired and sleep after high school too, we just never connected the dots or acted on it.
A trip to her primary care physician for some routine blood tests proved to be much more confusing than we could have anticipated. Taylor had hemoglobin around 8 mg/dL, platelet count ~30K and neutrophils (what were those???) at 800. We quickly learned how out of range these were and anxiously awaited some follow up testing which only confirmed something serious was wrong.
We were referred over to a local cancer center with that set of information in hand. None of it was real to us at the time but after the oncologist ordered the first bone marrow biopsy, the scope of what was in front of us changed quickly.
 BMB results were not very conclusive, but that information, along with the ongoing issues in the CBC, escalated our concern. The doctor was pointing to bone marrow failure and sketching out a venn diagram of aplastic anemia/MDS/PNH on a post-it-note. It was shocking and surreal to be at a cancer center and hear those words spoken about our 21-year-old daughter. We heard things like “cytopenia”, “immense amount of therapy and pharmaceuticals…”, “more testing”, “very rare, a couple cases per million” …
BMB results were not very conclusive, but that information, along with the ongoing issues in the CBC, escalated our concern. The doctor was pointing to bone marrow failure and sketching out a venn diagram of aplastic anemia/MDS/PNH on a post-it-note. It was shocking and surreal to be at a cancer center and hear those words spoken about our 21-year-old daughter. We heard things like “cytopenia”, “immense amount of therapy and pharmaceuticals…”, “more testing”, “very rare, a couple cases per million” …
All the while, Taylor completed her junior year of engineering school under these circumstances (maintained Dean’s List!!) and was weeks away from departing for a summer engineering internship.
Another biopsy was called for, this time an in-office procedure at the oncologist’s office. So much information was passed around, we missed the detail about how that procedure would go. The initial BMB was done in an outpatient surgical center under moderate sedation. Taylor was not a fan of the sedation; she was so tiny and anemic that the sedation affected her significantly. For the in-office procedure, we expected the same approach. We prepared by asking the staff for minimal sedation, but learned the plan was to use only local anesthesia with a light oral antianxiety medication if desired. Taylor toughed it through that procedure and the results confirmed an empty marrow (<10% cellularity) to go along with the tri-lineal cytopenia. The oncologist thought Taylor had Aplastic Anemia and said only 600–1000 cases were diagnosed in the US each year. He also indicated that he might see one AA patient every 5–10 years and was recommending we seek out specialists in the field to best handle Taylor at that point. The oncologists had colleagues from earlier in his career with more relevant experience and took the lead on finding the right path forward for Taylor. At the same time, we went to work trying to learn all we could about bone marrow failure and aplastic anemia. Scared the crap out of us. The oncologist connected us with the team at the Mayo Clinic in Phoenix. Fortunately, we live only 30 minutes from there. We have seen so many other patients and caregivers that must travel longer or temporarily relocate for treatment.
Immediately, the team at Mayo took ownership of Taylor’s case, and we gained confidence in the path they laid out for her. For AA, the first protocol is a matched sibling donor for stem cell transplant (this was not available for Taylor), second was to follow an immunosuppressive routine (ATG/cyclosporine), and third was an unrelated matched donor for HCST. Mayo identified a 10/10 matched donor in the worldwide database and placed a “hold” on that donor for Taylor while trying the IST routine. There were so many trying moments along the way, like reading 100.4˚F temp at an office visit and being checked into Mayo immediately for 36 hours of IV antibiotics or being in the room while a PICC line is inserted into your daughter’s heart.
While getting settled with Mayo, we consulted with NIH about the IST/ Eltrombopag clinical trial that showed promise for AA patients. The IST routine alone historically had limited short/mid-term success along with common relapse or clonal evolution problems. Eltrombopag had shown to improve the first responses in many patients. The NIH had recently published the Eltrombopag study in NEJM which allowed us to get the protocol at Mayo too. So that was our course of action. The weeks and months that followed were a blur of 3 to 5 days per week in the infusion clinic for blood testing, and red blood and platelet transfusions when called for (hemoglobin at 6 is tough to live with as all the readers of our story will know), all the while watching any blip or jump in numbers with excitement. This went on for 5–6 months until we realized there was no response to IST at for Taylor.
 This was not the 2017 holiday season our family hoped for. Another biopsy confirmed Taylor’s marrow was still empty and along with the tri-lineal cytopenia confirmed the situation was still dire and maybe progressing. This biopsy also revealed some cytogenic anomalies for the first time (del 7q). It was stem cell transplant time for Taylor. The diagnosis for Taylor was ultimately hypoplastic MDS, which apparently is a derivative, hidden or related outcome for a small portion of young aplastic anemia patients.
This was not the 2017 holiday season our family hoped for. Another biopsy confirmed Taylor’s marrow was still empty and along with the tri-lineal cytopenia confirmed the situation was still dire and maybe progressing. This biopsy also revealed some cytogenic anomalies for the first time (del 7q). It was stem cell transplant time for Taylor. The diagnosis for Taylor was ultimately hypoplastic MDS, which apparently is a derivative, hidden or related outcome for a small portion of young aplastic anemia patients.
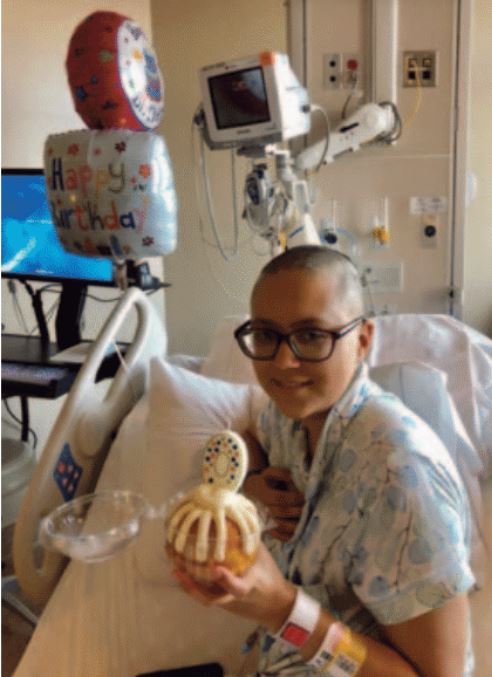
After a few weeks of mental prep and thorough health checks, we brought Taylor into the Mayo Clinic Phoenix transplant wing in mid-January 2018. The calendar-based transplant schedule provided was so basic yet communicated so effectively the day-by-day activity ahead, surreal to say the least. Day –7, –6, –5…counting down on the white board. Check the box for a shower, check the box for a walk around the pod, check the box for oral care…simple tasks in a normal life, but this was far from normal. We witnessed every minute of the process never leaving Taylor alone. Taylor says it was all a blur and fortunately for her not a lot of clear memories of the treatment duration. Nothing emotionally prepares parents for shaving your 21-year-old daughters head because long hair and multiple IV tubes are just not compatible. It was a relief to let go of the hair, and she looked great that way too! Chemo finished on Day –2, then a day of rest while Taylor’s anonymous donor was in their preparation routine halfway around the world and a Be the Match courier volunteer escorted the donation all the way to Phoenix. Those lifesaving stem cells arrived promptly on Day 0, January 25, 2018, and with a little ceremony the IV transfusion began. It was a very apprehensive day—would there be a reaction? Fortunately, uneventful, a mini-Bundt cake to celebrate her second additional birthday, and the healing process began! Taylor passed through the trough/nadir from the chemo and then a little blip in her numbers. Her white cell count went from zero to 0.1 overnight on about day 6 or 7 and steadily climbed thereafter. A few bouts of fevers and just general crappy feeling for Taylor. She was physically hanging in there, but the cabin fever was ramping up hard. By about day 10 Taylor pretty much had it with the whole process (can’t blame her), as her parents we wanted to ensure it would be a complication and stress-free transition home. We would have kept her in the pod until day 100 if we could, but Taylor was having none of that. We heard that most people get discharged at day 16–20. Taylor was discharged at day 13. Home we went. It was way more nerve wracking than when we took her home after her actual birth. This was adrenaline on adrenaline 24/7. Routine follow-ups were 3 to 4 days a week back the Ambulatory Infusion Clinic at Mayo for blood work and medication adjustments. We basically knew all the nurses, physician assistants and physicians so well at that point. Taylors numbers climbed steadily; blood product transfusions were a thing of the past. Now we were on to figuring out a way to nourish and hydrate Taylor when there really was no desire to take anything in. These times were tough. We are a fairly tech savvy family, but a reactivation of CMV virus lead us to have to give her “Party Ball” antiviral infusions at home 4 times a day for a month. A trainer came to the house and laid out the process we should follow by the supplies used at each step. Thorough hand wash, alcohol wipe, the flush syringes, clean the port, connect the IV, wait an hour, clean the port, clean the flush syringe, new port caps….daunting for sure, but routine in a few days. It was surreal to explain what we had to do to my co-workers. Fascinating and scary. We plugged along after the CMV was dealt with. Day 100 for Taylor was on Cinco De Mayo,  but there were no margaritas for any of us yet. Appetite and gastric issues continued; it was determined there was a bit of gastric aGVHD which introduced a new medication to the equation. All the while blood numbers showed Taylor to be a “normal” person at this point. A few months of the aGVHD treatment and gradually Taylor began to eat and drink at enough of a level to see her physically perk up and even put some weight back on. It was amazing to see her be able to get up a couple flights of stairs when only months earlier she would do it while seated on each step the whole way, one step at a time. Now she was bounding up the stairs. We took Taylor to Boston in July 2018 to visit family, see the Foo Fighters at Fenway Park, and attend the MDS Foundation Patient and Family Seminar. Taylor is unique at these conferences since she is so young in the MDS world. Later that summer, Taylor re-enrolled at ASU to complete her senior year of biomedical engineering. It was not always easy, always a small issue here or there that we completely lost our s**t over. Eventually, it was graduation day. Taylors’s life has been disrupted but she still has managed to achieve many personal goals.
but there were no margaritas for any of us yet. Appetite and gastric issues continued; it was determined there was a bit of gastric aGVHD which introduced a new medication to the equation. All the while blood numbers showed Taylor to be a “normal” person at this point. A few months of the aGVHD treatment and gradually Taylor began to eat and drink at enough of a level to see her physically perk up and even put some weight back on. It was amazing to see her be able to get up a couple flights of stairs when only months earlier she would do it while seated on each step the whole way, one step at a time. Now she was bounding up the stairs. We took Taylor to Boston in July 2018 to visit family, see the Foo Fighters at Fenway Park, and attend the MDS Foundation Patient and Family Seminar. Taylor is unique at these conferences since she is so young in the MDS world. Later that summer, Taylor re-enrolled at ASU to complete her senior year of biomedical engineering. It was not always easy, always a small issue here or there that we completely lost our s**t over. Eventually, it was graduation day. Taylors’s life has been disrupted but she still has managed to achieve many personal goals.
In early 2020 at the 2-year mark, we were introduced to Taylor’s selfless donor Andrezj from Poland. We have been able to communicate regularly with him using translate apps. We can’t thank Andrezj, his wife, and his children enough for completing the donation process on Taylor’s behalf. COVID and 2020 put further barriers in Taylors’s life. 2020 was another on-hold year, but onward and upward in 2021!
 Since transplant Taylor has been volunteering regularly with the Phoenix based Be the Match team and now will be joining National Marrow Donor Program (NMDP) and working with donors who have matched with patients from all over the world, preparing them to save more lives like her own. As parents we are so happy to see her get back to full life!
Since transplant Taylor has been volunteering regularly with the Phoenix based Be the Match team and now will be joining National Marrow Donor Program (NMDP) and working with donors who have matched with patients from all over the world, preparing them to save more lives like her own. As parents we are so happy to see her get back to full life!
We were very fortunate in many ways that my employer provided great insurance coverage for all procedures to this point and for what is still ahead of us. We realize not everyone is so fortunate to have access to great care networks, a matched donor, or the insurance to make it all possible. We are very grateful for all of that, to the scientists and pioneers in this field, and the current practitioners and support teams of this miracle cure.








